What’s the Link Between Gut Health and Gum Inflammation?
Imagine your body as a bustling ecosystem. Tiny microbes in your mouth and belly work in harmony—or chaos. When balance tips, trouble brews. Recent studies reveal a fascinating tie between what happens in your gut and the subtle ache in your gums. This isn’t just about bad breath or bleeding. It’s a window into whole-body wellness. Stick around as we unpack this duo and arm you with simple ways to thrive.
Understanding the Oral-Gut Axis
Your mouth and gut share more than meals. They form the oral-gut axis—a two-way street for bacteria and signals. Periodontal pathogens, those troublemakers behind gum swelling, don’t stay put. They hitch rides through saliva or blood to your intestines.
Research shows periodontitis disrupts gut flora. One study found salivary bacteria from inflamed gums alter gut diversity. This shift sparks dysbiosis—imbalanced microbes. In turn, a leaky gut lets toxins slip into your bloodstream, circling back to inflame oral tissues.
Think of it like a feedback loop. Poor oral hygiene invites harmful bugs. They migrate south, weakening your gut barrier. Hello, more inflammation everywhere. Experts now link this axis to broader issues like IBS or even rheumatoid arthritis.
| Key Statistics on Gut-Oral Health Links | Value | Source |
|---|---|---|
| U.S. adults over 30 with some periodontitis | 40% | UCSF Health |
| Periodontitis patients with gut dysbiosis correlation | High alpha diversity shift | Taylor & Francis Journal |
| Oral pathogens altering gut composition | Observed in animal models | Nature International Journal |
These numbers highlight urgency. Dysbiosis isn’t rare. It sneaks up, turning minor gum sensitivity into chronic woes.
How Poor Gut Health Fuels Gum Inflammation
Ever wonder why stress or diet swings hit your smile first? Blame the microbiome. An unhealthy gut ramps up cytokines—those fiery proteins. They travel systemically, targeting gum tissues. Chronic low-grade inflammation follows, eroding supporting bones.
Studies confirm it. Obese folks show gut changes heightening periodontitis odds. Fewer beneficial bacteria mean less protection against oral invaders like Porphyromonas gingivalis. This bug thrives in inflamed environments, worsening the cycle.
Pro tip: Fermented foods aren’t just trendy. They rebuild gut diversity, curbing oral fallout. Swap soda for kefir. Notice less puffiness around your teeth? That’s the axis at work.
Signs Your Gut Might Be Sabotaging Your Gums
Spotting the crossover early saves heartache. Watch for dual red flags. Bloating after meals? Paired with tender gums? Your gut may be calling shots.
Other clues: Persistent bad breath despite brushing. Or fatigue dragging you down, alongside loose teeth. These signal systemic strain. Research ties gut leaks to elevated oral antibodies, proving the breach.
Don’t ignore fatigue or irregular bowels. They often mask microbiome mayhem affecting your periodontal health. Track patterns in a journal. Share with your doc for tailored tweaks.
Actionable Steps to Nurture Gut and Oral Harmony
Ready to reset? Start small for big wins. Brush twice daily with fluoride paste. Floss like it’s your job—gently, but consistently. These basics starve oral villains before they gut-crash.
Boost fiber intake. Veggies like broccoli feed good gut bugs. Aim for 25 grams daily. Probiotics? Yogurt or supplements with Lactobacillus strains show promise in taming inflammation.
Hydrate smartly. Water rinses toxins, easing both ends. Cut sugar—it’s candy for bad bacteria. Exercise mildly; it stirs circulation, aiding microbial balance.
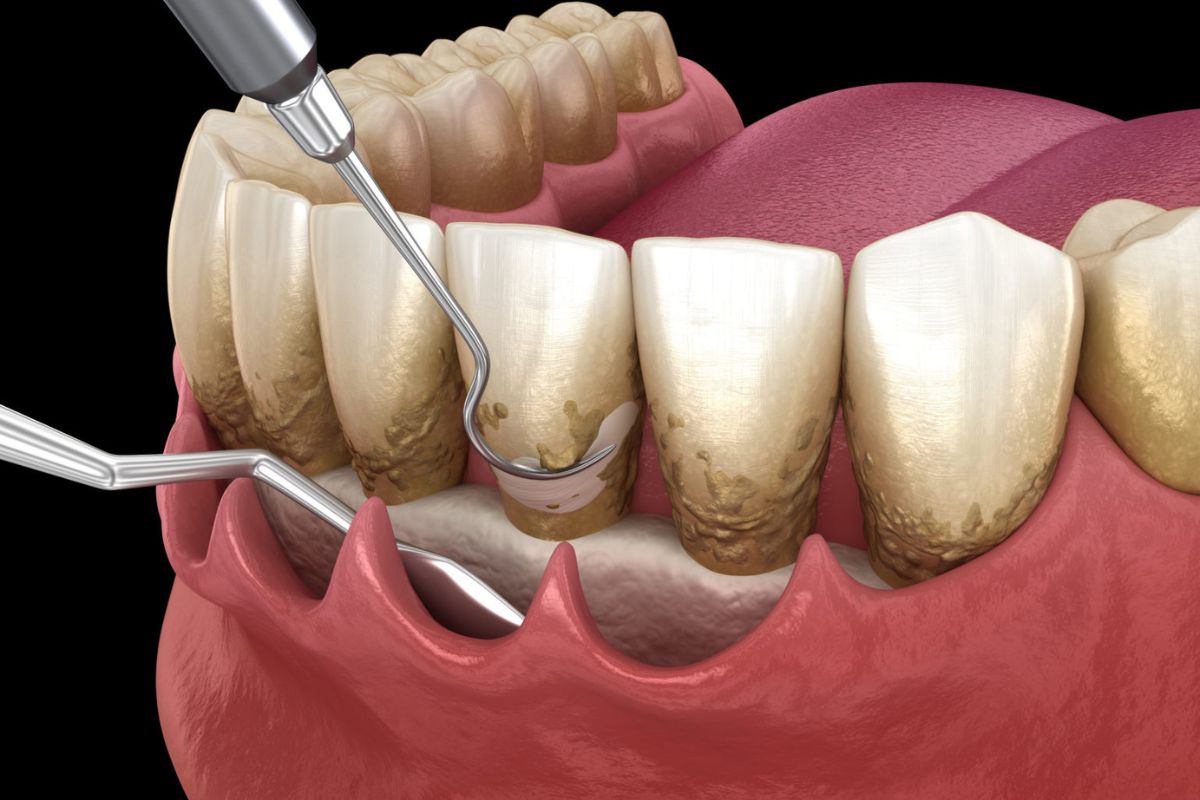
For deeper issues, scaling and root planing clears plaque buildup. If advanced, gum disease surgery restores stability. Always pair with gut-friendly habits for lasting results.
If persistent bleeding or recession bugs you, chat with a specialist. A periodontist in Arcadia, CA, can assess your unique setup. They blend local know-how with cutting-edge care.
Trending FAQs on Gut Health and Gum Inflammation
Curious minds search these often. Here’s what Google users ask most, with straight-talk answers based on fresh research.
- Can gum disease affect my gut health?
Yes. Harmful oral bacteria enter your bloodstream, disrupting gut flora. Studies link periodontitis to IBS flares via this migration. - How does gut health impact oral inflammation?
Dysbiosis triggers body-wide inflammation. Fewer good bacteria mean more cytokines hitting your gums, per Frontiers research. - What role does the microbiome play in gum disease?
It orchestrates immunity. Balanced microbes fight pathogens; imbalance invites overgrowth, leading to swelling and bone loss. - Are probiotics helpful for gum inflammation?
Often. Strains like Bifidobacterium reduce oral pathogens. Pair with diet for best results, as NYU studies suggest. - How does diet influence the gut-oral axis?
Fiber-rich foods promote diversity. Sugary diets starve good bugs, fueling inflammation on both fronts.
These insights empower you. Knowledge beats guesswork every time.
If you’re searching for a “periodontist near me,” look for one who gets the big picture. They should probe beyond symptoms, eyeing lifestyle ties like diet or stress. In areas like ours, pros tune treatments to daily realities—think pollen seasons tweaking allergies into oral sensitivities.
Your smile deserves a thriving foundation. Nurture that gut-oral bond today. Small shifts yield vibrant health tomorrow. Questions lingering? Reach out. Call (626)-445-8530 to schedule an appointment and reclaim your wellness. Here’s to balanced bugs and beaming grins.